Nighttime Nausea: Causes, Symptoms, and Effective Relief Tips
Waking up queasy—or feeling sick to your stomach the moment you lie down—can be unsettling, especially when it steals your sleep. Nighttime nausea is usually not a condition by itself. More often, it signals that something else is going on: reflux, digestion changes, medication effects, pregnancy, or stress/anxiety are common examples. (Cleveland Clinic, 2025; Mayo Clinic, 2019; Healthline, 2020)
Think of nausea like a check-engine light: it doesn’t always tell you exactly what’s wrong, but it does suggest looking for patterns and triggers. Below is a patient-friendly guide to what nausea at night can feel like, why it may worsen after bedtime, the most common causes, what tends to help, and when to seek care.
Quick Take—Why You Feel Nauseous at Night
Nighttime nausea is often associated with one or more common factors such as:
- Acid reflux/GERD, especially when lying flat after dinner
- Delayed stomach emptying (gastroparesis)
- Medication side effects (including effects related to dose timing)
- Pregnancy, even though it’s often nicknamed “morning sickness”
- Stress/anxiety, which can amplify physical sensations at bedtime
(Cleveland Clinic, 2025; Mayo Clinic, 2019; Healthline, 2020)
A common theme: nighttime tends to combine the “perfect conditions” for nausea—lying down, a day’s worth of meals, and fewer distractions.
Takeaway: Nighttime nausea is common and often linked to reflux, meal timing, medications, or stress.

What Does Nighttime Nausea Feel Like? (Common Symptoms)
Typical nausea symptoms
People describe nausea in different ways, but common symptoms include:
- Queasiness, “sour stomach,” or a rolling feeling in the stomach
- Loss of appetite
- Extra saliva, frequent burping, or bloating
- Gagging or dry heaving; sometimes vomiting
(Mayo Clinic, 2019)
Some people notice nausea as a wave that comes and goes; others feel a steady “off” sensation that makes it hard to fall asleep. Either way, try to connect the feeling to likely triggers.
Symptoms that may point to a specific cause
Certain “bonus symptoms” can be clues to what’s driving the nausea:
- Burning chest/throat, sour taste → possible GERD nausea at night
- Feeling very full after small meals → possible gastroparesis nausea
- Dizziness or a room-spinning sensation → possible vestibular issue/vertigo
- Headache with light sensitivity → possible migraine
(Mayo Clinic, 2019)
A simple way to describe the sensation for a clinician can be: is this mostly a stomach sensation, a dizziness sensation, or both?
Tip: Describing whether your nausea feels “stomach-based” or “dizzy-based” often helps guide next steps.

Why Nausea Often Gets Worse at Night
Lying flat may make reflux more likely
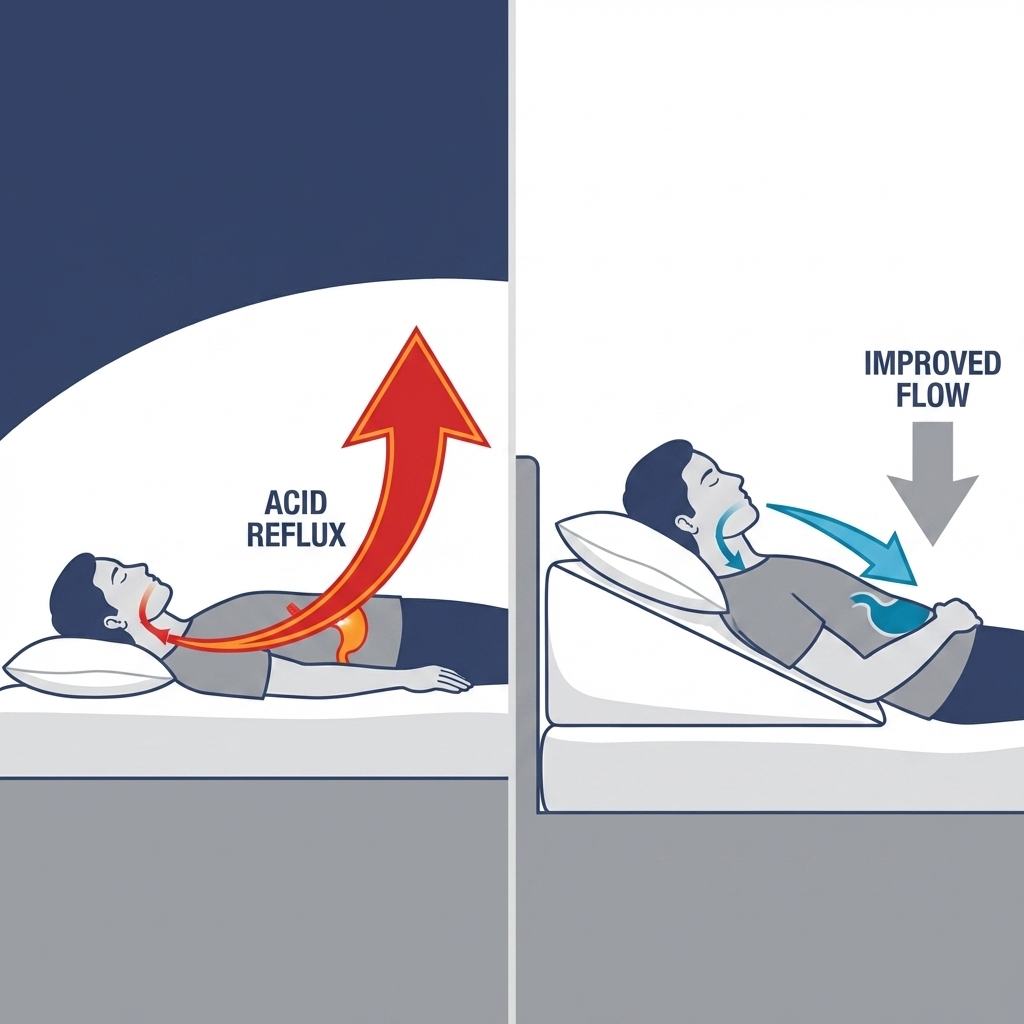
When you lie down, gravity stops helping keep stomach contents where they belong. That can make it easier for acid to move upward, irritating the esophagus or throat and sometimes triggering nausea, coughing, or a sour taste. (Healthline, 2020)
If you’re exploring reflux patterns, this comparison may help: LPR vs. GERD (reflux that affects the throat).
Evening meals and digestion timing
A heavier dinner or late snack can leave more food and acid sitting in the stomach at bedtime. Digestion may feel slower in the evening or after lying down, so “too full” sensations can feel more intense at night—especially for people prone to reflux or delayed emptying. (Healthline, 2020)
Related reading: how big meals can trigger acid reflux.
Medication timing
Some medications are more likely to cause nausea when taken at night—particularly if they irritate the stomach, are taken without food, or are followed by lying down soon afterward. (Healthline, 2020; Mayo Clinic, 2019)
Anxiety can feel louder at bedtime
At night, your environment gets quieter—so body sensations and worries can feel “turned up.” Many people say their mind starts scanning for symptoms as soon as the lights go out, which can intensify stress-related nausea. (Healthline, 2020)
Bottom line: Lying down, large or late meals, medication timing, and stress can all make nighttime nausea more noticeable.
The Most Common Causes of Nighttime Nausea
More than one cause can happen at the same time. For example, reflux plus stress plus a new medication can combine into a perfect storm.
GERD (acid reflux)
- How it can cause nausea: stomach acid flows upward and irritates the esophagus/throat. (Mayo Clinic, 2019)
- Clues: heartburn, sour taste, throat clearing, cough that’s worse at night, symptoms after spicy/fatty foods
- Why it may be worse at night: lying flat after dinner can make reflux more likely
Clinicians often hear versions of: “I’m fine during the day, but as soon as I lie down, I feel sick.” That bedtime pattern is commonly seen with reflux.
If reflux is a recurring theme, these may help:
- Best sleep positions for acid reflux relief
- Chronic acid reflux and ENT effects (voice/throat)
- LPR vs. GERD (reflux that affects the throat)
Gastroparesis (delayed stomach emptying)
- How it can cause nausea: food remains in the stomach longer than normal, which can trigger fullness, bloating, and nausea. (Healthline, 2020)
- Clues: feeling full quickly, nausea after eating, abdominal bloating; sometimes vomiting undigested food
- Night pattern: symptoms may build after a day of meals, so evenings can feel worse
Medication side effects (or taking meds at night)
Many medications can trigger nausea—especially after a new start or dose change. Examples often linked with medication-related nausea include:
- Some antibiotics
- NSAIDs (nonsteroidal anti-inflammatory drugs)
- Opioids
- Some antidepressants
- Some blood pressure medications
(Healthline, 2020; Mayo Clinic, 2019)
Clues: nausea begins after a medication change, or it peaks after the nightly dose. Timing and formulation sometimes matter—so it’s usually better to ask a clinician or pharmacist than to stop a prescription abruptly.
Pregnancy (nausea can happen at any time)
Despite the nickname, “morning sickness” can occur in the evening or overnight, especially early in pregnancy. (Healthline, 2020)
Stress/anxiety
Stress can affect the gut through nervous system signaling and hormone changes. Some people notice bedtime nausea, appetite shifts, reflux flare-ups, or a “knot in the stomach” feeling when stress is high. (Healthline, 2020)
Low blood sugar (hypoglycemia)
Low blood sugar can cause nausea, especially if dinner was skipped or alcohol was involved.
- Clues: shakiness, sweating, fast heartbeat/palpitations, feeling weak along with nausea
(Mayo Clinic, 2019)
Migraines
Nausea is common with migraines, and migraines can occur at night or even wake people from sleep. (Mayo Clinic, 2019)
If headaches are part of your pattern, this comparison can help clarify symptoms: migraine vs. sinus headache.
Vestibular problems (vertigo/motion sensitivity)
Inner-ear or vestibular issues can cause nausea plus dizziness (including a room-spinning sensation), and symptoms can worsen when rolling over in bed or changing head position. (Mayo Clinic, 2019)
Related: BPPV vertigo vs. dizziness—what’s the difference?
Acute illness (food poisoning or stomach bug)
Foodborne illness and viral gastroenteritis often cause nausea/vomiting and may feel worse at night due to fatigue and dehydration risk. (Mayo Clinic, 2019)
Cyclic vomiting syndrome (less common but important)
This condition involves repeated episodes of severe nausea/vomiting with symptom-free stretches in between. It’s less common, but it’s a key possibility when patterns are intense and recurring. (Healthline, 2020; Mayo Clinic, 2019)
Related reading you might find helpful:
- Can sleep apnea make you nauseous in the morning?
Key idea: Multiple factors—from reflux and gastroparesis to migraines or vertigo—can contribute to nighttime nausea, sometimes all at once.
When to Seek Medical Care (Don’t Wait)
Call a clinician promptly if you have:
- Persistent nausea lasting more than about 1 week or frequent recurrence (Cleveland Clinic, 2025)
- Trouble keeping fluids down or signs of dehydration (very dark urine, dizziness) (Cleveland Clinic, 2025)
- Unexplained weight loss (Cleveland Clinic, 2025)
Seek urgent/emergency care if nausea comes with:
- Severe abdominal pain or chest pain
- Fainting, confusion, severe headache
- New neurologic symptoms (weakness, trouble speaking, vision changes)
- Vomiting blood
(Cleveland Clinic, 2025; Mayo Clinic, 2019)
If symptoms are severe, persistent, or come with red flags, prompt medical evaluation is important.

How Nighttime Nausea Is Evaluated (What to Expect at an Appointment)
Symptom history that helps
A clinician will often focus on patterns—because patterns point to causes. Helpful details include:
- Timing: after dinner vs. middle of the night vs. early morning
- Food triggers (spicy/fatty foods), alcohol, caffeine
- Complete medication and supplement list (and when you take each)
- Pregnancy possibility
- Stress level, sleep disruption, dizziness, headaches
(Mayo Clinic, 2019)
If you can describe a “typical night” (what you ate, when symptoms started, what made it better/worse), it can be surprisingly diagnostic.
Possible tests (depending on symptoms)
Evaluation varies based on the most likely cause and whether any red flags are present. Possibilities may include:
- A reflux-focused plan based on symptoms (or referral/testing if needed)
- Labs for dehydration, infection, pregnancy, or metabolic issues
- Imaging or specialist referral when symptoms suggest a more urgent condition
(Mayo Clinic, 2019)
Sharing clear timelines, triggers, and medication timing can speed up diagnosis and treatment planning.
Effective Relief Tips You Can Try Tonight
Common strategies for nighttime nausea focus on reducing triggers and helping the body feel steadier.
Position changes (especially if reflux is suspected)
- Many people find it helps to elevate the head of the bed (or use a wedge pillow).
- Avoid lying down soon after eating. (Healthline, 2020)
If you want a concrete target, try staying upright for a set time after dinner and note whether symptoms change. For more ideas, see best sleep positions for acid reflux relief.
Food and timing tweaks
- Smaller dinners may reduce “too full” nausea.
- Limiting common reflux triggers may help some people: fatty foods, spicy foods, chocolate, peppermint, and alcohol. (Healthline, 2020; Mayo Clinic, 2019)
- Consider earlier meals if late-night snacking seems to worsen symptoms. Related reading: how big meals can trigger acid reflux.
Hydration strategies
- If vomiting or diarrhea is present, small sips of water or oral rehydration solution are often better tolerated than large amounts at once. (Mayo Clinic, 2019)
Gentle “settle your stomach” options
- If nausea seems related to an empty stomach, a small bland snack (like crackers or toast) helps some people.
- Ginger (tea or lozenges) is a commonly used supportive option; ginger may not be suitable for everyone, including some people who are pregnant or taking certain medications.
Calm the nervous system
- Slow breathing, a short wind-down routine, dim lights, and less screen time may reduce the “amplified” feeling that can come with stress at bedtime. (Healthline, 2020)
Small changes to meal timing, sleep position, and wind-down habits can make nighttime nausea more manageable.

Treatments That May Help (OTC and Prescription Options)
Educational note: labels and interactions matter—especially for people who take multiple medications or have chronic conditions—so many people confirm options with a pharmacist or clinician.
Over-the-counter options (often used for reflux-related nausea)
- Antacids for fast, short-term relief
- H2 blockers or PPIs for more frequent reflux symptoms (Healthline, 2020; Mayo Clinic, 2019)
Prescription options (based on the cause)
Depending on what’s driving symptoms, a clinician may consider:
- Stronger acid-reducing therapy for GERD if OTC isn’t enough
- Antiemetics (anti-nausea medications) in appropriate situations (Cleveland Clinic, 2025)
- Prokinetic medications for gastroparesis in select cases (Healthline, 2020)
Addressing medication-induced nausea
When causes point back to medication effects, clinician-guided strategies can include:
- Adjusting timing (with food vs. without; morning vs. night)
- Considering a better-tolerated alternative when appropriate (Healthline, 2020)
Work with a clinician or pharmacist before starting, stopping, or changing any medication.
Long-Term Prevention (Reduce Recurrence)
Build an evening routine that lowers risk
If nighttime nausea is recurring, consistency helps with both prevention and pattern recognition:
- Regular meal timing
- A predictable cut-off time for snacks
- A sleep-position plan if reflux is a frequent trigger
Track patterns for 1–2 weeks
A simple log can be surprisingly useful:
- Dinner time and foods
- Alcohol/caffeine intake
- Stress level
- Medication timing
- Nausea severity and timing
Bringing that log to an appointment can speed up diagnosis. (Mayo Clinic, 2019)
Treat the underlying condition
Long-term improvement usually comes from addressing the root issue—whether that’s a GERD plan, migraine prevention, anxiety support, or medication adjustments. (Cleveland Clinic, 2025; Mayo Clinic, 2019)
Consistent routines plus targeted treatment of the root cause offer the best long-term relief.
FAQs About Nighttime Nausea
Is nighttime nausea usually GERD?
GERD is a common reason for nausea at night, but it isn’t the only one. Medications, stress, pregnancy, migraines, vestibular issues, and other conditions can also contribute. (Mayo Clinic, 2019; Healthline, 2020)
Why do I feel nauseous right when I lie down?
Lying flat may make reflux more likely. It can also intensify dizziness-related nausea in people with vestibular conditions. (Healthline, 2020; Mayo Clinic, 2019)
What should I eat (or avoid) before bed?
If reflux is likely, heavy, fatty, or spicy late meals are common triggers. (Healthline, 2020) You can also explore sleep-related contributors here: can sleep apnea make you nauseous in the morning?
When is nausea serious enough to see a doctor?
If it’s persistent, severe, causes dehydration, or comes with alarming symptoms (severe pain, neurologic symptoms), it warrants medical evaluation. (Cleveland Clinic, 2025; Mayo Clinic, 2019)
Can stress alone cause nausea at night?
Stress/anxiety can trigger or worsen nausea, and it often feels more noticeable at bedtime when the environment is quiet and the mind is less distracted. (Healthline, 2020)
If you’re unsure whether your symptoms fit GERD, migraine, vertigo, or something else, a clinician can help narrow it down.
Related Reading (Internal Links)
- Best sleep positions for acid reflux relief
- Chronic acid reflux and ENT effects (voice/throat)
- Can sleep apnea make you nauseous in the morning?
- LPR vs. GERD (reflux that affects the throat)
- How big meals can trigger acid reflux
- BPPV vertigo vs. dizziness—what’s the difference?
- Migraine vs. sinus headache
Conclusion and Next Step
Nighttime nausea is common, and many cases improve once the underlying cause is identified—whether that’s reflux/GERD, gastroparesis, medication side effects, pregnancy, stress/anxiety, migraines, or a vestibular issue. (Cleveland Clinic, 2025; Mayo Clinic, 2019)
If nausea is persistent, disruptive to sleep, or paired with warning signs (like dehydration, severe pain, neurologic symptoms, or vomiting blood), medical evaluation can help clarify the cause and rule out treatable problems.
Next step (CTA): Consider discussing your symptoms with a qualified healthcare provider. If you’d like support from our team, you can book an appointment with https://www.sleepandsinuscenters.com/ to review your symptoms and discuss next-step testing or treatment options.
Identifying your personal triggers and treating the root cause are the fastest routes to better nights.
Sources
- Cleveland Clinic. Nausea (updated 2025). https://my.clevelandclinic.org/health/symptoms/nausea
- Healthline. Nausea at Night: Causes, Treatment, Prevention (2020). https://www.healthline.com/health/nausea-at-night
- Mayo Clinic. Nausea: Causes (2019). https://www.mayoclinic.org/symptoms/nausea/basics/causes/sym-20050736
Medical Disclaimer
This article is for general education and is not a substitute for personalized medical advice, diagnosis, or treatment.
This article is for educational purposes only and is not medical advice. Please consult a qualified healthcare provider for diagnosis and treatment.
Don’t let allergies slow you down. Schedule a comprehensive ENT and allergy evaluation at Sleep and Sinus Centers of Georgia. We’re here to find your triggers and guide you toward lasting relief.







