Can a Sinus Infection Cause Shortness of Breath? Symptoms, Causes, and When to See a Doctor
Shortness of breath is not a common direct symptom of a sinus infection. If it happens with sinus symptoms, treat it as urgent and get medical care. Sinusitis typically causes facial pressure, congestion, and nasal drainage—not breathing trouble. Symptom overviews from Johns Hopkins Medicine and the NHS list congestion, facial pain/pressure, and thick nasal discharge as typical sinusitis symptoms, while shortness of breath is not considered a standard feature. [1][2]
If you’re wondering can a sinus infection cause shortness of breath, it’s safest to frame it this way: sinus symptoms and breathing symptoms can show up at the same time, but shortness of breath often points to something else (or a complication) that needs prompt evaluation.
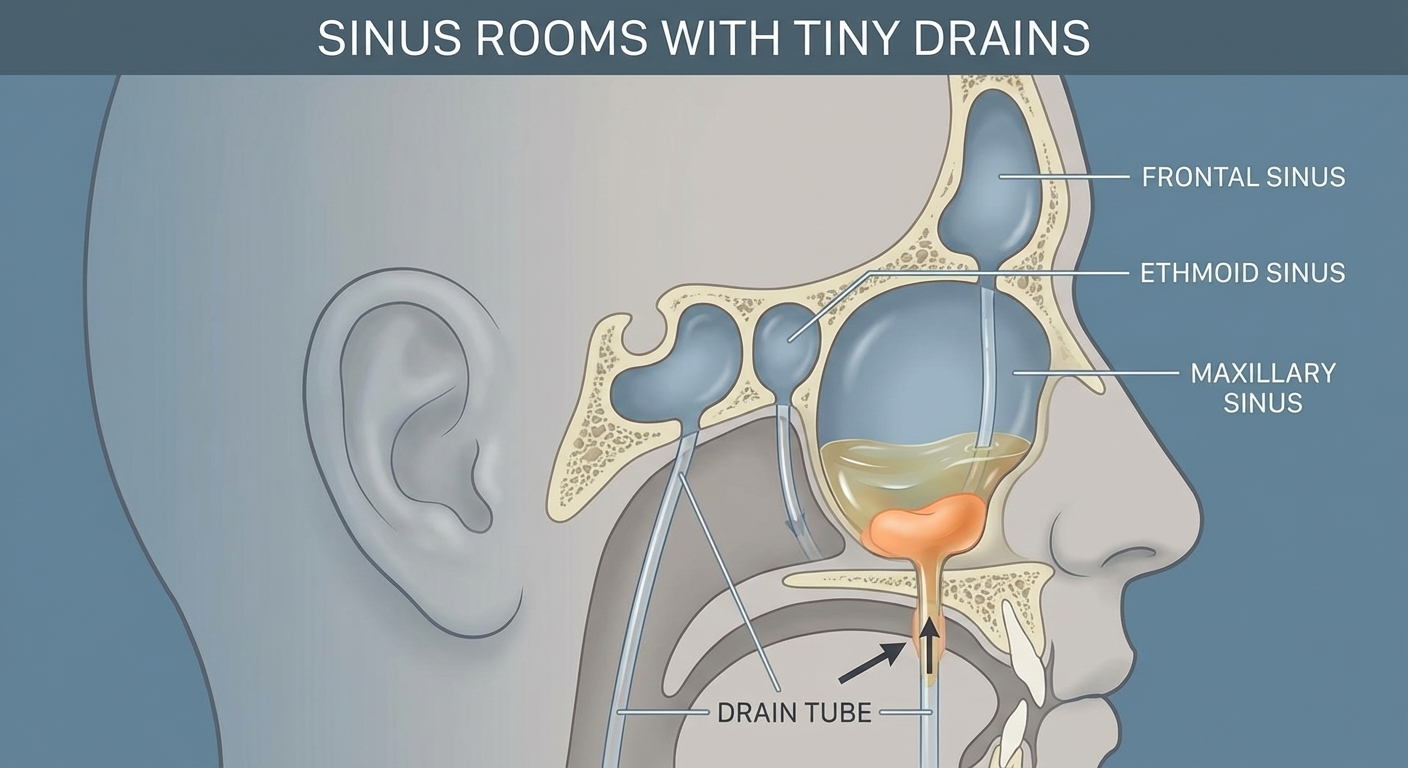
A helpful analogy: your sinuses are like small air-filled rooms with tiny drains. When the lining swells, the drains clog and pressure builds. That’s miserable—but it’s different from the lungs and airways, where true shortness of breath usually starts.
Quick Answer: Is Shortness of Breath a Sinus Infection Symptom?
Most of the time, no—sinusitis affects the air-filled spaces behind the cheeks, eyes, and forehead, and it typically causes:
- facial pressure or pain
- nasal congestion
- thick mucus or postnasal drainage [1][2]
Because shortness of breath usually involves the lungs, airways, or heart, shortness of breath with sinus symptoms should be evaluated promptly. [2]
What Is a Sinus Infection (Sinusitis)?
Sinusitis explained in plain language: Sinusitis (often called a sinus infection) is inflammation of the lining of the sinuses. When that lining swells, the normal drainage pathways can get blocked. Pressure builds, mucus can thicken, and drainage becomes impaired.
Many cases start after a routine cold: you feel stuffed up, drainage slows down, and the “rooms” (sinuses) don’t ventilate the way they normally do.
Acute vs. chronic sinusitis (why it matters):
- Acute sinusitis: Often starts after a cold and typically improves within days to a couple of weeks.
- Chronic sinusitis: Symptoms persist for a longer stretch (often weeks to months) or keep coming back.
If symptoms have lingered or recurred frequently, learn more on our chronic sinusitis page: https://sleepandsinuscenters.com/chronic-sinusitis
Bottom line: sinusitis means inflammation; it isn’t always a bacterial infection and often follows a cold or allergy flare.

Why Shortness of Breath Can Happen “With” a Sinus Infection (Even If It’s Not Caused by It)
Why it’s not a typical direct symptom: Sinuses are located in the face; shortness of breath generally reflects lower airway (lungs/bronchi) or cardiovascular issues. That’s why major medical resources describing sinus infection symptoms focus on nasal blockage, facial pressure, and thick discharge—not breathing difficulty. [1][2]
A quick location check that can help:
- Sinus symptoms tend to feel like pressure, congestion, thick discharge, reduced smell, and facial tenderness. [1][2]
- Breathing symptoms (shortness of breath, wheeze, chest tightness) more often suggest the lower airways or another process—and deserve timely evaluation. [2]
Common overlap reasons (sinus symptoms + breathing trouble):
- Postnasal drip → cough and throat irritation. Drainage can trigger coughing (often worse at night), throat clearing, and a “tight” or irritated upper-airway sensation. Example: you lie down, drainage pools in the throat, you cough repeatedly, and afterward you feel winded. Learn more: https://sleepandsinuscenters.com/blog/post-nasal-drip-causes-symptoms-and-effective-treatments
- Nasal blockage → mouth breathing and poor sleep. A blocked nose can lead to mouth breathing, dry throat, and disrupted sleep, which can heighten the sensation of air hunger.
- Allergies linking the nose and lungs. Allergies can inflame the nasal passages and sinuses—and in some people, they can also trigger asthma symptoms like wheeze or chest tightness. [3]
When it may signal a complication or separate condition: Sometimes, shortness of breath alongside sinus symptoms reflects a different illness at the same time, such as asthma flare, bronchitis, pneumonia, flu or COVID. Less commonly, it may be due to heart-related issues or a pulmonary embolism (especially with chest pain, fainting, or leg swelling). Related article: https://sleepandsinuscenters.com/blog/can-a-sinus-infection-lead-to-pneumonia
If breathing feels difficult, don’t wait to see if it passes—seek timely medical care.
Common Sinus Infection Symptoms (What You’d Usually Expect)
For a broader overview of sinus infection symptoms and related patterns, see: https://sleepandsinuscenters.com/symptoms-of-sinus-problems
Typical sinusitis symptoms:
- Facial pain/pressure/tenderness (cheeks, around eyes, forehead) [2]
- Nasal congestion (blocked nose) [2]
- Runny nose and/or thick green/yellow mucus [2]
- Reduced sense of smell [2]
- Headache [2]
- Ear pressure/fullness [2]
Other possible symptoms:
- Fever/high temperature (more common in acute cases) [2]
- Toothache [2]
- Bad breath [2]
- Cough, often worse at night due to drainage [2]
Symptoms that are not typical—and should raise concern: shortness of breath, chest pain/pressure, blue lips/face, confusion, severe weakness, swelling/redness around an eye, severe headache, or stiff neck should prompt urgent medical evaluation. [2]
Mucus color alone does not determine whether the infection is bacterial.
Causes and Risk Factors (Why Sinus Infections Start)
Most common causes:
- Viral upper respiratory infection (common cold) → swelling blocks drainage and triggers symptoms [2]
- Bacterial sinusitis → less common than viral; may be suspected when symptoms persist, worsen after initial improvement, or are severe [2]
If you’re trying to sort out sinus infection vs. cold patterns, this guide can help: https://sleepandsinuscenters.com/blog/sinus-infection-vs-cold-how-to-tell-the-difference
Contributors that can worsen sinus swelling:
- Allergies (seasonal or year-round) [3]
- Irritants (smoke, pollution, strong fragrances)
- Structural issues (deviated septum, nasal polyps)
- Chronic inflammation patterns that keep the lining irritated [1][3]
Reducing inflammation and improving drainage are the pillars of preventing and treating sinus symptoms.

What to Do If You Have Shortness of Breath With Sinus Symptoms (Action Steps)
This section is educational—not a substitute for care. Because shortness of breath can become serious quickly, it’s commonly treated as a symptom that needs timely medical attention.
When to call 911 / go to the ER now:
- Severe or worsening shortness of breath
- Difficulty speaking in full sentences
- Chest pain/pressure, fainting, confusion, bluish color
- New severe wheezing or, if you have a pulse oximeter and your readings are low, seek urgent care according to clinician guidance
When to seek same-day urgent care or a clinician visit:
- Mild but persistent shortness of breath
- Shortness of breath with fever, significant cough, or chest tightness
- A history of asthma, COPD, heart disease, or immune compromise
What you can do safely while you seek care:
- Rest and fluids
- Avoid smoke/strong odors
- If you already have a prescribed rescue inhaler for asthma, follow your established asthma action plan (avoid starting new medications without guidance)
If you’re unsure how urgent your symptoms are, err on the side of getting checked.
How Doctors Evaluate This Combination of Symptoms
Questions they’ll ask often cover timeline (cold → sinus symptoms → breathing symptoms), fever, chest pain, wheezing, exposure risks, asthma/allergy history, and current medications. It helps to share specifics such as: “I’m coughing mostly at night,” or “I feel chest tightness when I walk upstairs.”
Possible exams/tests may include vital signs and oxygen saturation, a lung exam (listening for wheezing or crackles), a nasal exam (sometimes endoscopy or imaging for persistent/recurrent sinusitis), and chest X-ray or viral testing when pneumonia/flu/COVID is suspected.
Clear details about your symptoms and timeline can speed diagnosis and treatment.

Treatment Options for Sinusitis (And What Helps vs. What Doesn’t)
Home care / symptom relief: The NHS describes common self-care approaches for sinusitis focused on symptom relief. [2] Options often include saline rinses or sprays (with proper technique and hygiene), OTC pain/fever relief (follow label directions), humidification and warm compresses, and adequate sleep and hydration.
When medications may be recommended: Depending on the cause and pattern of symptoms, a clinician may recommend nasal steroid sprays to reduce inflammation (often helpful when allergies contribute) [3], and antibiotics only when bacterial sinusitis is suspected; unnecessary antibiotics can cause side effects and contribute to resistance. [2]
For more on that decision-making, see: https://sleepandsinuscenters.com/blog/do-i-always-need-antibiotics-for-a-sinus-infection
If sinus problems keep returning: When symptoms are frequent or persistent, it may be worth exploring underlying contributors like allergies, chronic inflammation, or anatomy. Book an appointment: https://www.sleepandsinuscenters.com/appointments
Treat the cause, relieve the blockage, and reduce inflammation for the best long-term results.

Lifestyle Tips to Reduce Sinus Flares (And Protect Breathing)
Allergy control basics:
- Track triggers (pollen, dust, pets, mold)
- Use a consistent plan when allergies are confirmed [3]
Home environment tips:
- Reduce smoke exposure; consider HEPA filtration if helpful for your environment
- Keep indoor humidity balanced (very dry air can irritate; excess moisture can encourage mold)
Habits that help prevention:
- Hand hygiene during cold/flu season
- Stay hydrated
- Address chronic nasal obstruction—especially if it affects sleep quality
Small daily habits can lower flare-ups and make breathing feel easier.
When to See a Doctor for a Sinus Infection (Even Without Shortness of Breath)
Schedule a visit if symptoms last more than 10 days, worsen after initial improvement, or keep returning. [2] Also consider evaluation for severe facial pain, high fever, or worsening one-sided symptoms.
See a specialist (ENT) if you have frequent infections per year, symptoms that persist despite treatment, or possible structural contributors (polyps, deviated septum).
Timely care can prevent complications and shorten the course of illness.
FAQs
Can a sinus infection cause wheezing? Wheezing typically suggests lower-airway involvement (like asthma or bronchospasm). Sinusitis can coexist, but new or worsening wheeze should be assessed.
Is green mucus always a bacterial infection? Not always. Mucus color can change with viral inflammation, too. Persistence, severity, and the pattern of symptoms matter more than color alone. [2]
Can postnasal drip make you feel short of breath at night? Postnasal drip can trigger cough and throat irritation that feels like breathing is harder, particularly when lying down. True shortness of breath still deserves evaluation.
When is sinusitis considered serious? Red flags include breathing difficulty, eye swelling, severe headache, confusion, and high fever—seek urgent evaluation. [2]
Do allergies increase the risk of sinus infections? Yes. Ongoing nasal inflammation from allergies can contribute to blockage and increase sinusitis risk. [3]
References
1. Johns Hopkins Medicine – Sinusitis overview and symptoms: https://www.hopkinsmedicine.org/health/conditions-and-diseases/sinusitis
2. NHS – Sinusitis symptoms, self-care, and when to seek help: https://www.nhs.uk/conditions/sinusitis/
3. AAAAI – Sinusitis and allergy relationship: https://www.aaaai.org/conditions-and-treatments/library/allergy-library/sinusitis
This article is for educational purposes only and is not medical advice. Please consult a qualified healthcare provider for diagnosis and treatment.
Don’t let allergies slow you down. Schedule a comprehensive ENT and allergy evaluation at Sleep and Sinus Centers of Georgia. We’re here to find your triggers and guide you toward lasting relief.







